When a child has asthma, their inhaler isn’t just a tool-it’s their lifeline. But if the technique is off, that lifesaving medicine might never reach their lungs. Studies show that without a spacer and mask, kids under 8 deliver only 10-20% of the dose to their airways. That’s like trying to fill a glass with a漏斗 that’s half blocked. The good news? With the right technique, that number jumps to over 80%. And it’s not about buying the fanciest device-it’s about doing eight simple steps right.
Why Kids Need a Spacer and Mask
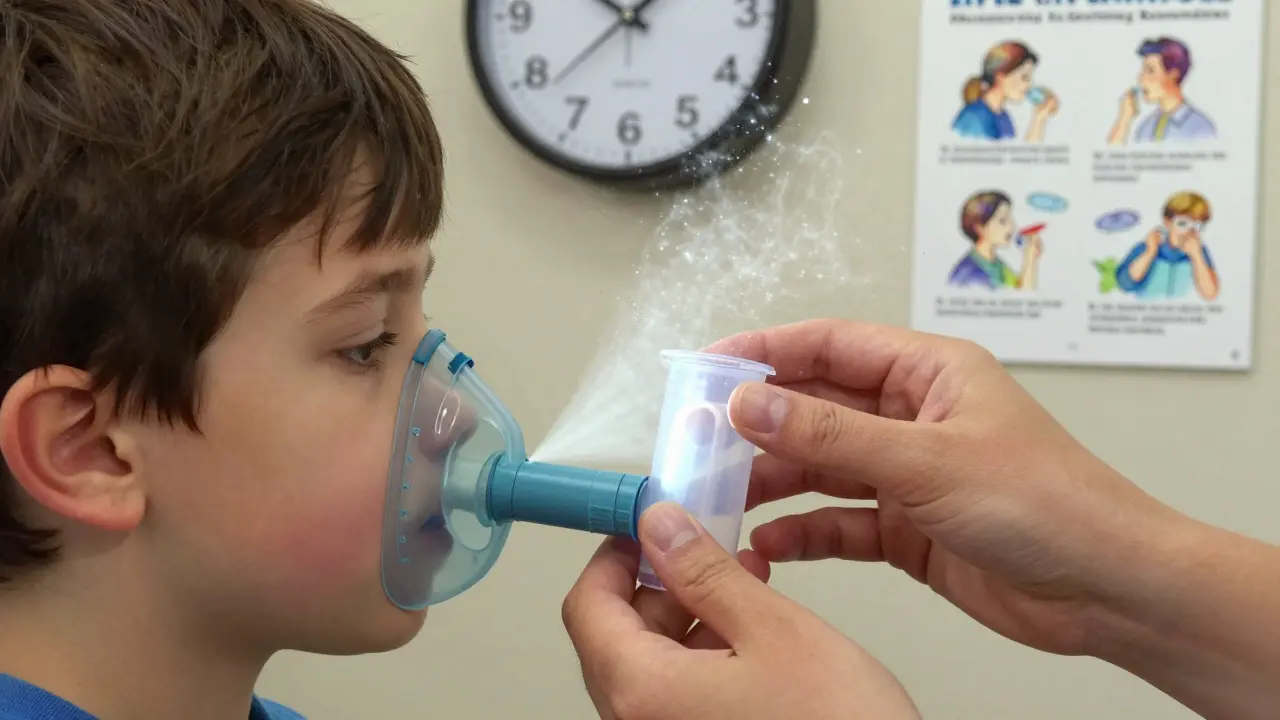
Young kids can’t time their breath with the puff. They cough, laugh, or pull away. That’s why a metered-dose inhaler (MDI) alone doesn’t work. A spacer-also called a valved holding chamber-holds the medicine in a chamber after it’s sprayed. Then, the child breathes it in slowly over several breaths. Add a face mask, and you don’t even need them to cooperate. The mask seals over nose and mouth, so no medicine escapes.
Research from Johns Hopkins and Children’s Hospital of Philadelphia shows that using a spacer with mask increases lung delivery from 12% to 78%. The difference? It’s not magic. It’s physics. The spacer stops the medicine from hitting the back of the throat. Instead, it floats gently in the chamber, waiting for the child to breathe it in naturally.
Choosing the Right Spacer and Mask Size
Not all spacers are made the same. For infants under 12 months, use a spacer with a volume of 150-350 mL. Toddlers (1-3 years) need 350-500 mL. Preschoolers (3-8 years) do best with 500-750 mL. Too small? The medicine bounces back. Too big? It’s hard to hold steady.
Mask fit matters just as much. The edge should sit from the bridge of the nose to the bottom of the chin-not covering the cheeks. If you can see skin around the edges, it’s too loose. A 2022 audit found that 63% of parents used masks that were too big or too small. That’s why some brands include sizing guides. Look for one that shows where the mask should sit. If yours doesn’t, use a ruler. Measure from the nose to chin. Match that to the mask size.
The 8-Step Technique (For Kids Under 8)
Follow this sequence every time. Skipping even one step cuts effectiveness by 30%.
- Shake the inhaler for 10 seconds. Don’t just give it a quick shake. You need to fully mix the medicine. A 2021 study showed 42% of parents shook for less than 5 seconds. That means uneven doses.
- Attach the spacer and mask. Make sure the valve clicks into place. Check that the mask isn’t cracked or warped. A damaged spacer can leak up to 20% of the dose.
- Place the mask firmly on the face. Seal it around the nose and mouth. Use both hands. One hand on the mask, one on the inhaler. No gaps. If the child is crying or squirming, wait. Don’t rush.
- Press the inhaler once. One press. One puff. Don’t press twice. Don’t hold it down. The medicine shoots into the spacer. You’ll hear a click or see a mist.
- Let the child breathe in slowly through the mask. For infants and toddlers, they need 5-10 normal breaths. No deep inhales. Just regular breathing. You’ll see the valve in the spacer move with each breath. That’s good.
- Wait 30-60 seconds before removing the mask. This lets the medicine settle. Remove it too soon, and you lose up to 15% of the dose.
- Wait 1-3 minutes between puffs. If they need a second puff, wait at least a minute. Rushing puffs overwhelms the lungs and wastes medicine.
- Wash the spacer weekly. Use warm water and a drop of dish soap. Don’t towel-dry. Air-dry upside down. Static buildup from dry spacers can reduce delivery by 28%. The UK Inhaler Group says washing isn’t always needed-but for most homes, it is.
What Changes as Kids Get Older
By age 5 or 6, many kids can switch from a mask to a mouthpiece. But only if they can seal their lips around it and hold their breath.
Here’s how to transition:
- Start with the mouthpiece while still using the spacer.
- Teach them to breathe out fully before putting the mouthpiece in.
- Press the inhaler, then take one slow, deep breath in.
- Hold that breath for 10 seconds.
- Then breathe out slowly.
Studies show this single-breath method delivers 69% of the dose-better than the mask for older kids. But if they can’t hold still or seal their lips? Go back to the mask. No shame. Technique beats age.
Common Mistakes (And How to Fix Them)
Parents aren’t alone. Even experienced caregivers mess up. Here are the top errors and how to fix them:
- Not shaking the inhaler long enough. Solution: Set a 10-second timer on your phone. Do it every time.
- Mask not sealed. Solution: Use a mirror. If you see fogging around the edges, it’s leaking. Adjust pressure.
- Too many puffs too fast. Solution: Space them out. Use a timer. One puff. Wait. Then next.
- Washing with a towel. Solution: Hang the spacer upside down after washing. Let air do the work.
- Using expired inhalers. Solution: Write the date on the canister when you open it. Most last 200 puffs. After that, even if it sprays, the medicine is weak.

How to Get Kids to Cooperate
Resistance is normal. A survey of 1,243 parents found that 78% of kids initially fight the mask. Here’s what works:
- Use masks with characters. Superheroes, animals, or cartoon faces help. One parent said, “My daughter only takes her inhaler if the mask has Paw Patrol.”
- Make it a game. “Let’s blow out birthday candles” before the puff. Or “Let’s see how many breaths we can take like a dragon.”
- Let them hold the spacer. Kids feel in control when they can press the inhaler themselves (with help).
- Practice without medicine. Do the steps with just the spacer and mask. No puff. Just breathing. Make it routine.
One mom on Asthma.com shared: “We practiced every night before bed. No medicine. Just breathing in and out through the mask. After two weeks, she didn’t flinch when I gave her the real one.”
When to Call the Doctor
Even with perfect technique, asthma can flare. Call your pediatrician if:
- Your child still wheezes after two puffs.
- You notice more than two rescue inhaler uses in a week.
- Their lips or fingernails turn blue.
- They’re too breathless to talk or walk.
And if you’re unsure about your technique? Ask for a video review. Hospitals like CHOP and Nationwide Children’s now offer telehealth check-ins where you record yourself giving the inhaler. One 2023 study found this cut emergency visits by 47%.
What’s New in 2026
Smart spacers are here. The FDA cleared the first one in 2023-a device that beeps when the child breathes too fast or too shallow. It connects to an app and gives real-time feedback. Early data shows kids using these improve technique by 33% in just four weeks.
Also, telehealth is changing the game. More than 60% of pediatric asthma clinics now ask parents to send short videos of inhaler use. No more guessing. Just clear, visual proof.
But here’s the truth: None of this matters if you skip the basics. A washed plastic bottle with a mask can work just as well as a $50 spacer-if the steps are done right. As one pulmonologist put it: “Technique is 10 times more important than the brand.”
Can I use a spacer without a mask for my 4-year-old?
No. Children under age 5 cannot reliably seal their lips around a mouthpiece. Using a spacer without a mask will let most of the medicine escape through the nose or mouth. Always use a properly sized face mask for kids under 8. The mask ensures the medicine goes into the lungs, not the air.
How often should I wash the spacer?
Wash the spacer once a week with warm water and a drop of mild dish soap. Do not use a towel to dry it. Let it air-dry upside down. Static buildup from dry spacers can block up to 28% of the medicine. Weekly washing keeps the chamber clean and the dose accurate. If you skip this, your child may get less medicine than prescribed.
Is it okay to use a spacer with a dry powder inhaler?
No. Dry powder inhalers (like Advair Diskus or Pulmicort Turbuhaler) require a strong, fast breath to pull the powder into the lungs. Children under 8 cannot generate enough airflow. Spacers are designed for metered-dose inhalers (MDIs), which spray medicine as a mist. Never use a spacer with a dry powder inhaler-it won’t work and may damage the device.
My child coughs after using the inhaler. Is that normal?
A little cough is normal, especially if the medicine hits the throat. But if they cough a lot, it may mean they’re not using the spacer correctly. Make sure the mask is sealed and they’re breathing slowly. Also, rinse their mouth with water after each use to reduce throat irritation. If coughing continues, check the technique or talk to your doctor.
How do I know if the inhaler is empty?
Most inhalers have a counter that shows how many puffs are left. If yours doesn’t, write the date you opened it on the canister. Most MDIs last for 200 puffs. After that, even if it sprays, the medicine is weak or gone. Never guess. If you’re unsure, replace it. A half-empty inhaler can be worse than none-it gives false confidence.


Nicole Blain
March 18, 2026 AT 11:14Kathy Underhill
March 18, 2026 AT 17:32Prathamesh Ghodke
March 20, 2026 AT 02:11Stephen Habegger
March 21, 2026 AT 07:04Kendrick Heyward
March 22, 2026 AT 08:49Melissa Starks
March 22, 2026 AT 12:44Lauren Volpi
March 23, 2026 AT 01:27Melissa Stansbury
March 23, 2026 AT 01:38